Electrophysiology (EP) Collaboratory
Overview
Convened and co-hosted by MDIC with the Stanford Center for Arrhythmia Research, the Electrophysiology Collaboratory (EP Collaboratory) is dedicated to advancing the science, evidence, and clinical infrastructure needed to bring electrophysiology innovation to patients — faster and in the United States.
Bringing together device manufacturers, clinical investigators, FDA, CMS, academic medical centers, professional societies, and patient advocates, the EP Collaboratory operates in the pre-competitive space where shared challenges benefit from a shared solution. Our work spans the full spectrum of EP innovation: from the earliest human experience with novel devices to the generation of clinical evidence that informs regulatory approval and patient access.

Vision
Our vision is to serve as the home for pre‑competitive regulatory science in electrophysiology. We bring together broad perspectives, disciplines, and expertise across the innovation lifecycle to provide shared tools, foster collaboration, and support a clear path from early development to patient access.
Impact
The EP Collaboratory envisions an ecosystem within which electrophysiology innovations are imagined, developed, tested, and delivered to patients in the United States with optimized quality and efficiency.
We seek to enable participation in early‑stage device research across a wide range of clinical settings, including academic medical centers, integrated health systems, and high‑volume community practices.
Through strengthening site readiness and evidence generation, the Collaboratory supports industry confidence in conducting early feasibility studies in the United States and promotes the generation of evidence that is robust, reproducible, and suitable for regulatory and payer review.
The EP Collaboratory brings together a broad and diverse coalition of stakeholders to:
Reduce barriers to conducting early feasibility studies (EFS)
Reduce barriers to conducting early feasibility studies (EFS) in the United States by developing practical tools, playbooks, and site infrastructure.
Generate consensus through the AF Ablation Academic Research Consortium
Generate consensus on clinical trial design, safety endpoints, and efficacy measures for atrial fibrillation therapies through the AF Ablation Academic Research Consortium.
Support Multi‑Stakeholder Dialogue on Evidence Development
Convene multi‑stakeholder discussions to surface shared evidence challenges and support readiness for formal regulatory interactions, consistent with established FDA processes.
Build a network of EP Pioneer Institutions
Build a self-sustaining clinical site network of EP Pioneer Institutions ready to enroll first-in-human and EFS patients within 90 days of protocol finalization.
Reduce barriers to EP Clinical Research
Develop key performance indicators to monitor and communicate progress on reducing barriers to U.S.-based EP clinical research.
EP Collaboratory Projects
The Collaboratory advances its mission through two flagship initiatives, each targeting a distinct stage of the EP innovation lifecycle.
Early Feasibility Studies (EFS) Initiative
The FDA’s 2013 EFS IDE Guidance created a pathway for conducting small-scale, first-in-human device studies in the United States. Despite strong regulatory support, the majority of EP early feasibility studies continue to be conducted overseas — not due to FDA barriers, but because of site-level operational challenges including contract complexity, budget unpredictability, and long startup timelines.
The EFS Initiative addresses these root causes directly through a comprehensive, freely available toolkit and a growing network of EP Pioneer Institutions committed to 90-day protocol-to-enrollment performance.
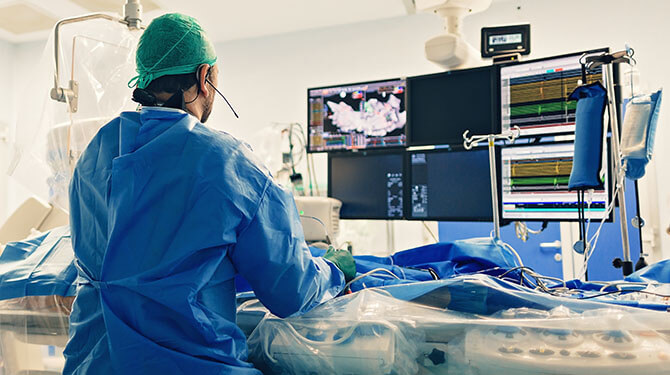
Atrial Fibrillation Ablation Academic Research Consortium (AF-ARC)
Establishing consensus on safety endpoints, efficacy measures, and clinical trial design for atrial fibrillation ablation therapies.
The landscape of AF ablation therapy has expanded dramatically — from catheter-based pulmonary vein isolation to pulsed field ablation, surgical approaches, and emerging hybrid therapies. Yet clinical trial design in this space remains inconsistent, with heterogeneous endpoint definitions, variable follow-up durations, and disparate patient selection criteria that limit cross-study comparability and complicate regulatory and payer review.
The EFS Initiative addresses these root causes directly through a comprehensive, freely available toolkit and a growing network of EP Pioneer Institutions committed to 90-day protocol-to-enrollment performance.
What is a Collaborative Community?
A collaborative community is a continuing forum in which private- and public-sector members, which can include the FDA, work together on medical device challenges to achieve common objectives and outcomes. They are convened by interested stakeholders and may exist indefinitely, produce deliverables as needed, and tackle challenges with broad impacts.
The EP Collaboratory is among the first FDA-recognized Collaborative Communities in electrophysiology. To learn more about the FDA Collaborative Community program, visit the FDA Collaborative Communities webpage.
FAQ
The EP Collaboratory is open to any organization or individual with a stake in electrophysiology innovation. This includes device manufacturers, clinical investigators and academic medical centers, community and integrated health system EP programs, FDA and CMS, professional societies (including HRS), patient advocacy organizations, and CROs. MDIC membership is not required.
No. MDIC serves as the convener of the EP Collaboratory, and non-MDIC members are welcome to participate fully. Certain MDIC member benefits — including priority access to working groups and toolkit development — are available to MDIC members.
EP Pioneer Institutions are clinical sites that have committed to the operational infrastructure needed to achieve 90-day protocol-to-first-patient enrollment timelines for EFS studies. Qualifying sites have identified dedicated study management personnel, secured institutional buy-in from key stakeholders (IRB, contracts, budget, technology), and adopted the MDIC EFS toolkit. Reach out to the EP Collaboratory team to begin the qualification process.
Sponsors can engage through the EFS Explorer to identify site partners, participate in working groups, or request facilitated informal conversations with FDA through the Collaboratory network. Sponsors at any stage of EP device development — from early design through IDE — are encouraged to connect early.
All EP Collaboratory resources — including the EFS Playbook, CTA template, budgeting template, site selection tools, FDA engagement checklist, and EFS Explorer — are freely available here. The toolkit is currently in preview mode, with a full public launch planned for June 2026.
Join Us!
Whether you are a clinical site looking to build EFS infrastructure, a sponsor navigating the IDE pathway, or a researcher shaping the next generation of AF ablation trial design — there is a place for you at the table.
To join the EP Collaboratory or learn more, contact the MDIC EP Collaboratory team below
EP Collaboratory Leadership
Paul Wang, MD, Stanford Center for Arrhythmia Research
Co-Chair, EP Collaboratory; Director, Stanford Center for Arrhythmia Research
Eileen Mihas, MDIC
Center Head, Center for Evidence and Patient Engagemenet
Jonah Golder, MDIC
Senior Project Manager
Learn more about Early Feasibility Studies at MDIC
To learn more about MDIC’s Early Feasibility Studies (EFS) initiative reach out to efs@mdic.org.